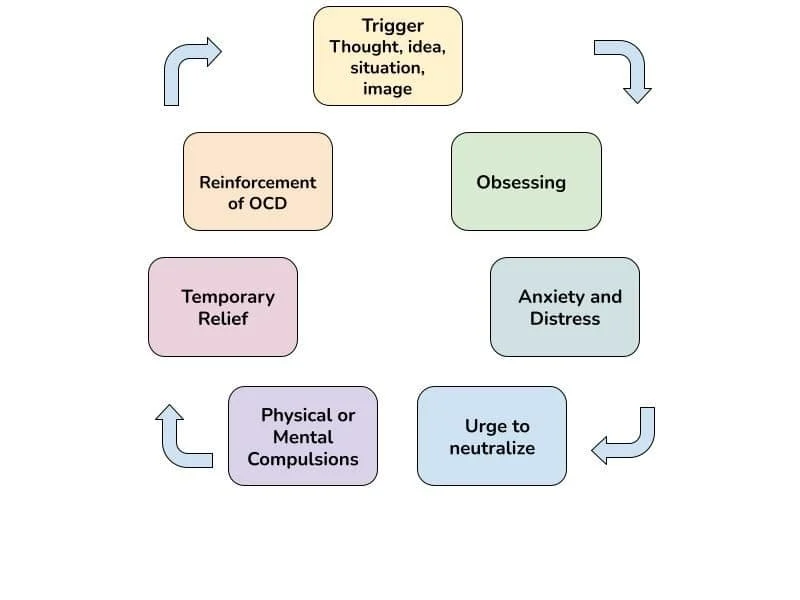
Obsessive compulsive disorder (OCD) is when a person gets caught in a cycle of obsessions and compulsions. Obsessions are unwanted thoughts, images, or urges that may be extreme or disturbing. The obsessions are accompanied by uncomfortable feelings. These obsessions occur over and over again and feel outside of the person’s control.
Common obsessions include:
- Contamination
- Perfectionism
- Harm coming to oneself or other
- Loss of Control over one’s actions
- Unwanted intrusive thoughts, usually violent or sexual
- Religious obsessions
Compulsions are excessive, repetitive behaviors or “mental acts” (e.g., thought suppression, counting, or praying) that a person uses to try to neutralize or make their obsessions or distress go away.
Common compulsions include:
- Frequent, excessive washing and cleaning
- Frequent, excessive checking (e.g., that the door is locked and the oven is off)
- Repeating
- Mental compulsions (e.g., counting, praying, reviewing)
- Frequent, excessive reassurance seeking (e.g., asking “Are you sure I’m going to be OK?”
- Avoiding situations that might trigger obsessions
Disorders relating to OCD:
- Hoarding disorder (HD), in which individuals collect and keep a lot of items that clutter living spaces, keep spaces from being used as intended, and cause distress or problems in day-to-day activities.
- Body dysmorphic disorder (BDD), in which individuals are very preoccupied with one or more aspects of their physical appearance, and perform repetitive compulsive behaviors to fix, hide, inspect, or obtain reassurance about the disliked aspects.
- Body-focused repetitive behaviors (BFRBs), in which individuals perform repeated, compulsive self-grooming behaviors that result in damage to their body. BFRBs include excoriation disorder (skin picking) and trichotillomania (hair pulling).
Research suggests that OCD involves problems in communication between the front part of the brain and deeper structures of the brain. These brain structures use a neurotransmitter (basically, a chemical messenger) called serotonin. Pictures of the brain at work also show that, in some people, the brain circuits involved in OCD become more normal with either medications that affect serotonin levels (serotonin reuptake inhibitors, or SRIs) and/or cognitive behavior therapy (CBT).
GETTING TREATMENT
OCD can only be diagnosed by a licensed mental health professional.
The most effective treatments for OCD are cognitive behavioral therapy (CBT) and/or medication. More specifically, the most effective and evidence-based treatments are a type of CBT called exposure and response prevention (ERP).
OCD assessment and ERP are provided as part of your treatment.